'Nip the virus in the bud': How Germany showed Europe the way on coronavirus testing
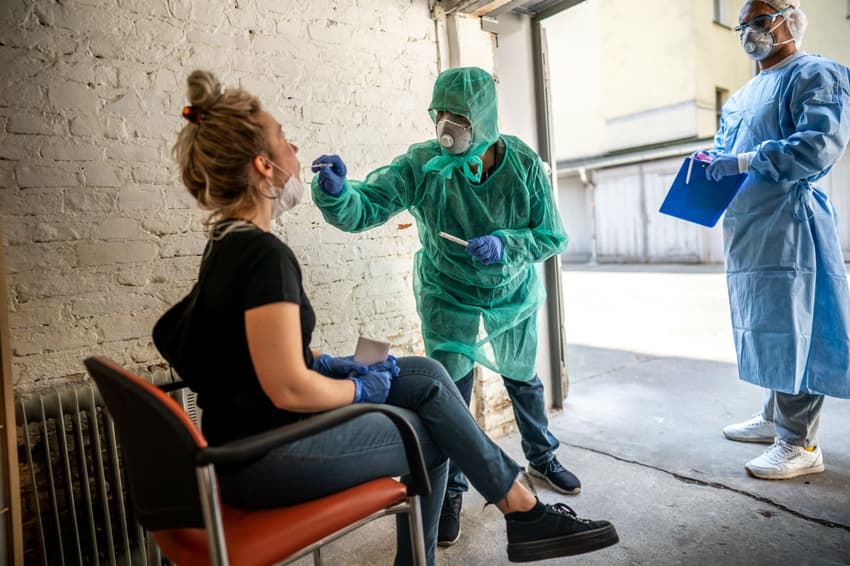
It’s taken other countries in Europe months to develop an adequate coronavirus testing regime needed to combat the pandemic. Rachel Stern examines how Germany managed it much sooner and how the country continues to lead the way.
On a sunny Friday afternoon in mid-June, Berliners enjoyed picnics in public parks, gathered at outdoor street markets and filled the outdoor terraces of restaurants.
But Hannah, a 21-year-old trainee nurse in the German capital, kicked off the weekend by starting a two-week quarantine in her flat, having just discovered she had been infected with Covid-19 after coming into contact with an acquaintance confirmed to have the disease.
“I had no symptoms, but I still tested positive,” Hannah told The Local.
When a friend told her she was infected, Hannah quickly arranged for a test at the hospital where she works and received the results the same day.
In other countries governments have been heavily criticised for not providing rapid testing for healthcare workers or indeed the general population, even those with symptoms - a factor scientists believe exacerbated the spread of the disease.
But since the first outbreak of coronavirus Germany has made testing a priority, and now as lockdowns ease and public life reopens testing has become a crucial weapon in the fight against any resurgence of the virus.
The country’s continual effort to test its residents for the coronavirus is considered one of the key factors which has led to its low per capita case numbers and low death rate, and spared its medical system from a crippling overload experienced in other European countries.
It continues to be one of the few countries in Europe with an “open public testing” policy meaning even asymptomatic people can have access to tests. In contrast countries like France and the UK are only testing those with symptoms or those who have come into contact with anyone infected.
READ ALSO: Germany to expand coronavirus testing for people without symptoms
By mid-June it had carried out over five million tests out of its population of 83 million people, according to the Robert Koch Institute.
As of Friday June 26th, Germany has had over 196,000 confirmed coronavirus cases, over 176,760 which are reported to have recovered, according to data from Johns Hopkins University. There have also been 8,940 deaths, well below the numbers seen in France, Italy, Spain and the UK.
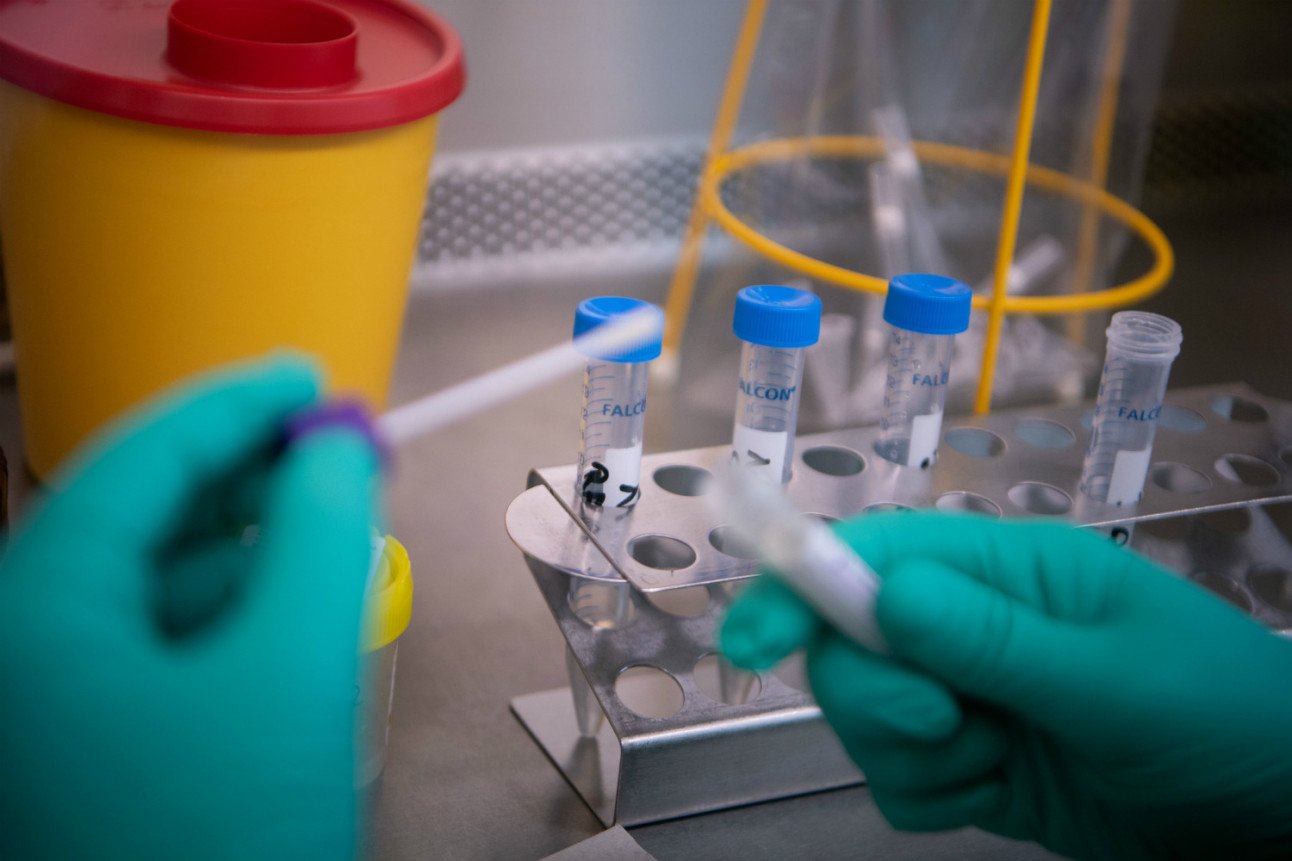
Testing for the novel coronavirus in a lab. Photo: DPA
Taking action from the beginning
Germany’s success with getting its testing system up and running was down to several factors.
Firstly it acted quickly when the first cluster emerged in the country back in January.
Germany’s first coronavirus case was detected on January 27th at a car parts manufacturer just outside of Munich, also marking the first incident of human to human transmission of the virus in Europe.
The case was traced back to an employee who had recently visited her parents in Shanghai and brought back the virus.
After confirming the virus, local health officials also ordered tests for 40 people who had been in contact with the infected employees, including colleagues and family members. Importantly the company, Wabasco, paid for 139 Covid-19 tests.
This quick-fire testing to isolate the cluster at such an early stage of the outbreak was considered crucial by experts to prevent the kind of outbreak and knock-on effects on the health service seen in other countries.
“If this cluster of infections in Bavaria hadn’t been discovered, then Germany could have had a situation like that in Italy,” Professor Jonas Schmidt-Chanasit, the chair of virology at the Bernhard Nocht Institute for Tropical Medicine, told The Local.
The example set in Bavaria was copied throughout Germany as infections spread to all 16 states.
“Infections were quickly registered and their contacts quickly reached,” so that they could be tested, said Schmidt-Chanasit.
It was exactly the kind of procedure recommended by the WHO, which other European countries struggled to put in place and only began to roll out once lockdowns were eased in May and June. The test was developed domestically by coronavirus expert Dr. Christian Drosten of Berlin’s renowned Charité university clinic.
At the peak of the epidemic in Germany, the week beginning March 30th - Germany carried out 408,000 tests a week, according to data from the Robert Koch Institute.
From the beginning of the outbreak Germany has relied on “PCR tests”, which detect viral RNA even before antibodies form or symptoms - which can take up to 14 days to show - are present.
READ ALSO: '200,000 tests a day': Germany pushes to expand coronavirus testing
Following the outbreak of SARS-CoV-2, as the virus is scientifically known, in Wuhan, China in December 2019, Drosten and his team of researchers got to work.
As soon as their Chinese colleagues made the genome sequence available, they were able to roll out the test which would not only be available for use by the end of January in Germany, but also worldwide.
Although not everything went smoothly in the early days of the epidemic in Germany.
Initially public health insurance companies would only pay for a test if someone showed systems of the virus.
Part of the rationale was that it was in the middle of flu season and, as such, a lot of German residents exhibited typical respiratory symptoms.
Some also reported challenges acquiring a test at the beginning.
Ali, a 34-year-old digital marketing executive who suspected he had Covid-19, was initially refused a test in a Berlin clinic because he didn’t show enough symptoms, but was able to eventually get one after “legal pressure” from his employer.
“The costs were by no means covered by the health insurance company, so my employer paid around €270,” Ali told The Local.
Things have changed since then with the German government realising it paid in the long run to invest in testing notably by covering costs that might have dissuaded members of the public from taking a test.
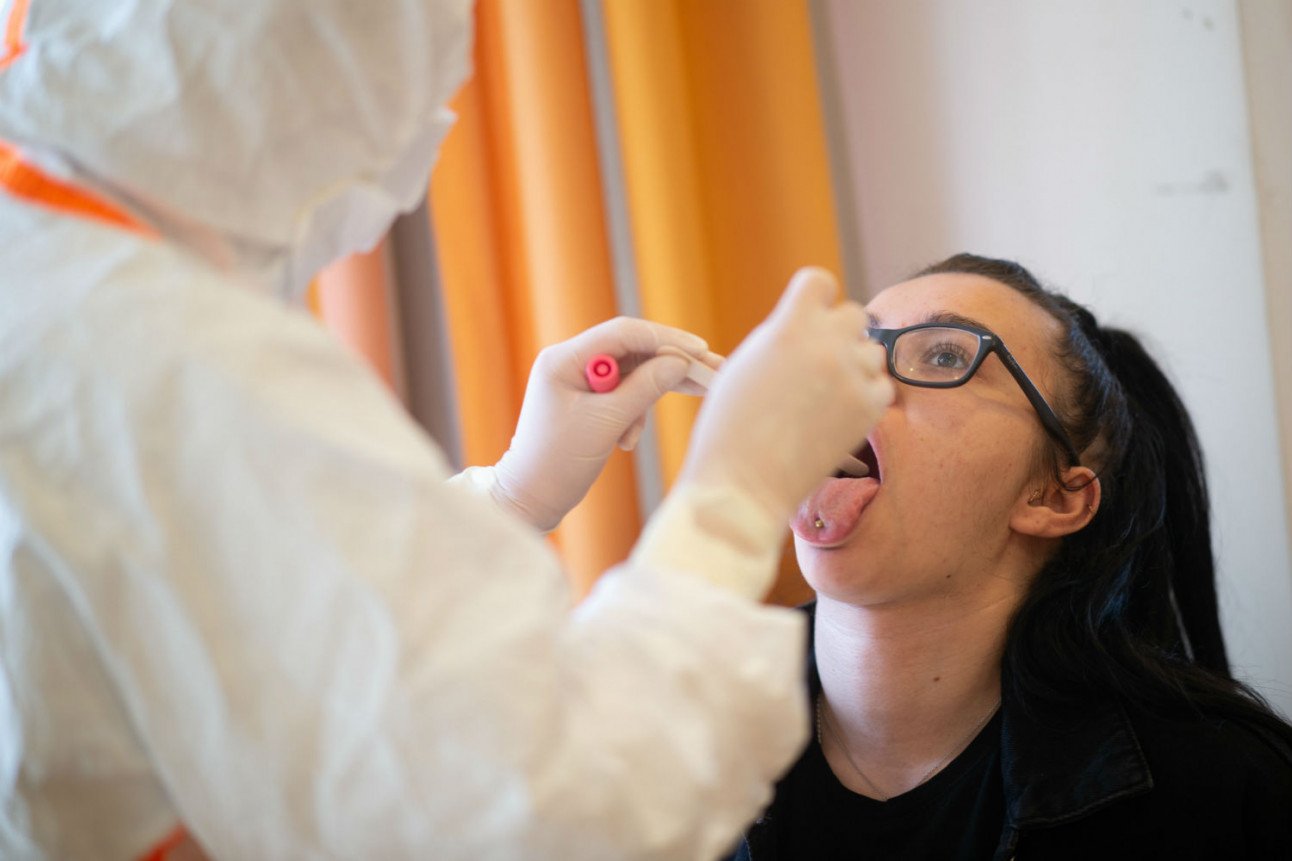
A woman receives a test in the coronavirus 'hotspot' of Heinsberg. Photo: DPA
Health Minister Jens Spahn of Chancellor Angela Merkel’s centre-right Christian Democrats said in June “It is much more expensive to test too little than to test too much."
Spahn was speaking after the German the Health Ministry announced that the country’s public health insurance would cover the roughly €50 test for anyone who suspected they might have coronavirus, even if they didn’t show symptoms.
The cost of all tests since May 15th would be covered, the ministry announced, for both the publicly and privately insured in Germany, and for any official testing centre or location.
READ ALSO: Germany plans to test everyone admitted to hospitals and nursing homes
Germany’s pharmaceutical industry played its part
Not everything came down to policy.
One of the reasons Germany was able to dramatically up its testing regime was that it could rely on its pharmaceutical industry.
While the coronavirus plunged Germany into its worst recession since World War II, its medical diagnostics industry - the largest in Europe - boomed due to an increased demand for testing.
A full 65 out of the 100 members of the Association of German Diagnostics Industry (VDGH) offer “corona tests and associated products”, a large number of them centering on standard PCR-Tests. Others often so-called Schnelltests (rapid tests), which give an immediate result but questions remain about their accuracy.
“The German government decided for an early, comprehensive and goal-oriented testing strategy,” said the VDGH during a presentation entitled ‘Why Germany is at the top of testing’ on June 12th.
READ ALSO: Germany ramps up coronavirus testing to 500,000 a week
Following the large coronavirus outbreak in February, Philipp Freese’s first thought was how to improve testing for the coronavirus.
His company PharmGenomics had focused on screenings for colon cancer, but it quickly shifted gears, developing an at-home PCR test (CoronaScreen) from genetic information which had already been published, and testing its 17 employees.
“It was pretty apparent that the pandemic would rapidly spread,” said Freese, whose wife comes from the district of Heinsberg, one of Germany’s original coronavirus hotspots.
“We decided that we have to help fight the pandemic and focus on this topic,” said Freese, who is raising the funds to finance the tests through a crowdfunding campaign dubbed #CrowdBeatsCorona. “We would lose our scarce time if we did not follow the trend.”
‘A blended approach’
According to the World Health Organisation (WHO), testing is a crucial tool in stemming the spread of the coronavirus, but must be part of a comprehensive approach which also includes quarantining confirmed and suspected cases for two weeks, ensuring sufficient capacity in the health care system such as beds and ventilators, and enforcing social distancing measures.
“Germany has been organized, they continued to test at high rates, they continued with tracking and tracing despite challenges,” a WHO spokesperson told The Local.
“They have activated the public health and social measures and implemented the comprehensive and blended approach as recommended by WHO,” the spokesperson added.
That comprehensive approach meant the battle against the epidemic wasn’t all about the testing strategy in Germany.
For a start the strict lockdown imposed across the country is credited with saving many lives and the government also moved to bolster its health system.
By mid-March, when the country counted slightly more than 11,000 confirmed cases and 27 deaths, it announced a plan to double its 25,000 hospital beds with respiratory care capacity.
They set aside enough space to not only accept severely ill patients from Germany, but also coronavirus patients from neighbouring EU countries when their own hospitals lacked capacity and supplies.
Ana, a nurse who works in intensive care at a hospital near Cologne, told The Local that while protective medical equipment (PPE) ran low, it never ran out and Germany had far more ventilators available to the worst-off Covid-19 patients that other countries.
'Nip the virus in the bud'
Widespread testing has so far helped Germany avoid a second wave of new infections as it transitions from a strict lockdown by crucially helping to identify and isolate new clusters such as the one that emerged at a meat-packing plant in North Rhine-Westphalia.
Out of 6,140 employees tested at the plant, 1,553 are confirmed to have been infected with coronavirus. The plant was immediately closed and a new local lockdown imposed on the whole district.

Tönnies, the slaughterhouse where a corona outbreak occurred in June. Photo: DPA
Further widespread testing in the area will continue, especially in care homes. In addition, everyone in the district is allowed to voluntarily undergo testing free of charge if they want to. If the numbers "remain low", the lockdown will be lifted.
Testing has also slowed smaller outbreaks that could have otherwise spiralled outside of control. At a residential complex in Berlin’s trendy Friedrichshain district, 44 people were confirmed to be infected with the virus on Wednesday June 24th.
The local health department arranged for testing - even for asymptomatic residents - after a contact person was identified.
“Among the people tested positive for Covid-19 by the health department, there are also children attending schools and day care centres...They affected facilities were informed immediately,” said the health department authorities, pointing out that immediate testing would occur at these locations.
"We want to nip the virus in the bud," said Health Minister Spahn.
Germany now has the capacity in its labs to carry out up to one million tests a week, Susanne Glasmacher, a spokesperson for the Robert Koch Institute, told The Local.
Of the tests which have been conducted, one percent have come back positive, “a very good result in international comparison,” said Glasmacher.
READ ALSO: Coronavirus outbreak in Germany is 'under control' says health minister
The test capacity in Germany has progressively grown larger since the start of the outbreak. By March 9th, there were 28 laboratories in Germany processing results, with a total of 7,115 tests carried out per week.
By June 15th, Germany counted 138 such labs, and had the capacity to carry out 166,445 tests per day, meaning capacity was nearly twice the number of actual tests being carried out.
But testing only works with tracing and Germany has 400 coronavirus call centres where operators field calls from people worried they might have contracted the virus after coming into contact with a person who tested positive.
They not only put them in touch with medical personnel to arrange for a test themselves, but - working with 21,000 tracers throughout the country - aim to track down every person the positive person has come into contact with and alert them.
Germany is also armed with a new voluntary coronavirus warning app, which can measure whether smartphone users have come closer than about two meters to an infected person for over 15 minutes.
They can then quickly seek out a test.
The success of testing also relies on those people who are positive going into a two-week quarantine, even if they have no symptoms.
Quarantine rules
Germany has strict punishments for those who flout the rules.
Violation of quarantine could in extreme cases result in a maximum prison sentence of up to two years or a steep fine. The health authorities check the quarantine by calling the affected person's home to talk to the patient and check how they are doing.
But not everything is perfect with Germany’s testing strategy.
Despite all of its resources, hotlines and testing centres for the coronavirus often remain closed on weekends, or after hours.
While large metropolitan centres are equipped with several makeshift centres and drive-in testing centres - which can accept patients after they are referred by local health authorities - more rural areas have less resources.
Amr Aswad, a virology researcher at Berlin's Free University, told The Local that the system for testing in Germany was working "very well" but that Germany could make an even greater push to test more asymptomatic people.
"There is a case to be made for testing more asymptomatic people, particularly in situations where a large number of people are gathered, even if they are observing social distancing," said Aswad.
"It's hard to say for sure but I think this could help stop the chain of transmission in its tracks early on."
Testing is 'building block'
The pandemic - and concerns about it - are still far from over in Germany as the recent outbreaks detailed above show.
As of Sunday June 21st, the so-called R-Wert or reproductive value, had shot up from 1.79 to 2.88 following the recent outbreaks.
What’s clear is that Germany, thanks to its well-established testing strategy set up right from the outset, appears well-placed to be able to prevent a second wave.
“Testing is a big building block,” said Schmidt-Chanasit. “It's very important as Germany goes from general blanket measures to specific ones. Testing plays a very important role in ensuring success.”
Schmidt-Chanasit said that such a comprehensive testing strategy of identifying contacts of an infected person - whether co-workers, schoolmates or acquaintances - is the way forward.
“As soon as a contact person arises, there must be a lot of testing,” said Schmidt-Chanasit.
“Now and in the future.”
Confronting Coronavirus: This article is part of a new series of articles in which The Local's journalists across Europe are taking an in-depth look at the responses to different parts of the crisis in different countries; what's worked, what hasn't, and why.
This article has been supported by the Solutions Journalism Network, a nonprofit organisation dedicated to rigorous and compelling reporting about responses to social problems.
The SJN has given The Local a grant to explore how different countries are confronting the various affects of the coronavirus crisis and the successes and failures of each approach.
Comments
See Also
On a sunny Friday afternoon in mid-June, Berliners enjoyed picnics in public parks, gathered at outdoor street markets and filled the outdoor terraces of restaurants.
But Hannah, a 21-year-old trainee nurse in the German capital, kicked off the weekend by starting a two-week quarantine in her flat, having just discovered she had been infected with Covid-19 after coming into contact with an acquaintance confirmed to have the disease.
“I had no symptoms, but I still tested positive,” Hannah told The Local.
When a friend told her she was infected, Hannah quickly arranged for a test at the hospital where she works and received the results the same day.
In other countries governments have been heavily criticised for not providing rapid testing for healthcare workers or indeed the general population, even those with symptoms - a factor scientists believe exacerbated the spread of the disease.
But since the first outbreak of coronavirus Germany has made testing a priority, and now as lockdowns ease and public life reopens testing has become a crucial weapon in the fight against any resurgence of the virus.
The country’s continual effort to test its residents for the coronavirus is considered one of the key factors which has led to its low per capita case numbers and low death rate, and spared its medical system from a crippling overload experienced in other European countries.
It continues to be one of the few countries in Europe with an “open public testing” policy meaning even asymptomatic people can have access to tests. In contrast countries like France and the UK are only testing those with symptoms or those who have come into contact with anyone infected.
READ ALSO: Germany to expand coronavirus testing for people without symptoms
By mid-June it had carried out over five million tests out of its population of 83 million people, according to the Robert Koch Institute.
As of Friday June 26th, Germany has had over 196,000 confirmed coronavirus cases, over 176,760 which are reported to have recovered, according to data from Johns Hopkins University. There have also been 8,940 deaths, well below the numbers seen in France, Italy, Spain and the UK.

Testing for the novel coronavirus in a lab. Photo: DPA
Taking action from the beginning
Germany’s success with getting its testing system up and running was down to several factors.
Firstly it acted quickly when the first cluster emerged in the country back in January.
Germany’s first coronavirus case was detected on January 27th at a car parts manufacturer just outside of Munich, also marking the first incident of human to human transmission of the virus in Europe.
The case was traced back to an employee who had recently visited her parents in Shanghai and brought back the virus.
After confirming the virus, local health officials also ordered tests for 40 people who had been in contact with the infected employees, including colleagues and family members. Importantly the company, Wabasco, paid for 139 Covid-19 tests.
This quick-fire testing to isolate the cluster at such an early stage of the outbreak was considered crucial by experts to prevent the kind of outbreak and knock-on effects on the health service seen in other countries.
“If this cluster of infections in Bavaria hadn’t been discovered, then Germany could have had a situation like that in Italy,” Professor Jonas Schmidt-Chanasit, the chair of virology at the Bernhard Nocht Institute for Tropical Medicine, told The Local.
The example set in Bavaria was copied throughout Germany as infections spread to all 16 states.
“Infections were quickly registered and their contacts quickly reached,” so that they could be tested, said Schmidt-Chanasit.
It was exactly the kind of procedure recommended by the WHO, which other European countries struggled to put in place and only began to roll out once lockdowns were eased in May and June. The test was developed domestically by coronavirus expert Dr. Christian Drosten of Berlin’s renowned Charité university clinic.
At the peak of the epidemic in Germany, the week beginning March 30th - Germany carried out 408,000 tests a week, according to data from the Robert Koch Institute.
From the beginning of the outbreak Germany has relied on “PCR tests”, which detect viral RNA even before antibodies form or symptoms - which can take up to 14 days to show - are present.
READ ALSO: '200,000 tests a day': Germany pushes to expand coronavirus testing
Following the outbreak of SARS-CoV-2, as the virus is scientifically known, in Wuhan, China in December 2019, Drosten and his team of researchers got to work.
As soon as their Chinese colleagues made the genome sequence available, they were able to roll out the test which would not only be available for use by the end of January in Germany, but also worldwide.
Although not everything went smoothly in the early days of the epidemic in Germany.
Initially public health insurance companies would only pay for a test if someone showed systems of the virus.
Part of the rationale was that it was in the middle of flu season and, as such, a lot of German residents exhibited typical respiratory symptoms.
Some also reported challenges acquiring a test at the beginning.
Ali, a 34-year-old digital marketing executive who suspected he had Covid-19, was initially refused a test in a Berlin clinic because he didn’t show enough symptoms, but was able to eventually get one after “legal pressure” from his employer.
“The costs were by no means covered by the health insurance company, so my employer paid around €270,” Ali told The Local.
Things have changed since then with the German government realising it paid in the long run to invest in testing notably by covering costs that might have dissuaded members of the public from taking a test.

A woman receives a test in the coronavirus 'hotspot' of Heinsberg. Photo: DPA
Health Minister Jens Spahn of Chancellor Angela Merkel’s centre-right Christian Democrats said in June “It is much more expensive to test too little than to test too much."
Spahn was speaking after the German the Health Ministry announced that the country’s public health insurance would cover the roughly €50 test for anyone who suspected they might have coronavirus, even if they didn’t show symptoms.
The cost of all tests since May 15th would be covered, the ministry announced, for both the publicly and privately insured in Germany, and for any official testing centre or location.
READ ALSO: Germany plans to test everyone admitted to hospitals and nursing homes
Germany’s pharmaceutical industry played its part
Not everything came down to policy.
One of the reasons Germany was able to dramatically up its testing regime was that it could rely on its pharmaceutical industry.
While the coronavirus plunged Germany into its worst recession since World War II, its medical diagnostics industry - the largest in Europe - boomed due to an increased demand for testing.
A full 65 out of the 100 members of the Association of German Diagnostics Industry (VDGH) offer “corona tests and associated products”, a large number of them centering on standard PCR-Tests. Others often so-called Schnelltests (rapid tests), which give an immediate result but questions remain about their accuracy.
“The German government decided for an early, comprehensive and goal-oriented testing strategy,” said the VDGH during a presentation entitled ‘Why Germany is at the top of testing’ on June 12th.
READ ALSO: Germany ramps up coronavirus testing to 500,000 a week
Following the large coronavirus outbreak in February, Philipp Freese’s first thought was how to improve testing for the coronavirus.
His company PharmGenomics had focused on screenings for colon cancer, but it quickly shifted gears, developing an at-home PCR test (CoronaScreen) from genetic information which had already been published, and testing its 17 employees.
“It was pretty apparent that the pandemic would rapidly spread,” said Freese, whose wife comes from the district of Heinsberg, one of Germany’s original coronavirus hotspots.
“We decided that we have to help fight the pandemic and focus on this topic,” said Freese, who is raising the funds to finance the tests through a crowdfunding campaign dubbed #CrowdBeatsCorona. “We would lose our scarce time if we did not follow the trend.”
‘A blended approach’
According to the World Health Organisation (WHO), testing is a crucial tool in stemming the spread of the coronavirus, but must be part of a comprehensive approach which also includes quarantining confirmed and suspected cases for two weeks, ensuring sufficient capacity in the health care system such as beds and ventilators, and enforcing social distancing measures.
“Germany has been organized, they continued to test at high rates, they continued with tracking and tracing despite challenges,” a WHO spokesperson told The Local.
“They have activated the public health and social measures and implemented the comprehensive and blended approach as recommended by WHO,” the spokesperson added.
That comprehensive approach meant the battle against the epidemic wasn’t all about the testing strategy in Germany.
For a start the strict lockdown imposed across the country is credited with saving many lives and the government also moved to bolster its health system.
By mid-March, when the country counted slightly more than 11,000 confirmed cases and 27 deaths, it announced a plan to double its 25,000 hospital beds with respiratory care capacity.
They set aside enough space to not only accept severely ill patients from Germany, but also coronavirus patients from neighbouring EU countries when their own hospitals lacked capacity and supplies.
Ana, a nurse who works in intensive care at a hospital near Cologne, told The Local that while protective medical equipment (PPE) ran low, it never ran out and Germany had far more ventilators available to the worst-off Covid-19 patients that other countries.
'Nip the virus in the bud'
Widespread testing has so far helped Germany avoid a second wave of new infections as it transitions from a strict lockdown by crucially helping to identify and isolate new clusters such as the one that emerged at a meat-packing plant in North Rhine-Westphalia.
Out of 6,140 employees tested at the plant, 1,553 are confirmed to have been infected with coronavirus. The plant was immediately closed and a new local lockdown imposed on the whole district.

Tönnies, the slaughterhouse where a corona outbreak occurred in June. Photo: DPA
Further widespread testing in the area will continue, especially in care homes. In addition, everyone in the district is allowed to voluntarily undergo testing free of charge if they want to. If the numbers "remain low", the lockdown will be lifted.
Testing has also slowed smaller outbreaks that could have otherwise spiralled outside of control. At a residential complex in Berlin’s trendy Friedrichshain district, 44 people were confirmed to be infected with the virus on Wednesday June 24th.
The local health department arranged for testing - even for asymptomatic residents - after a contact person was identified.
“Among the people tested positive for Covid-19 by the health department, there are also children attending schools and day care centres...They affected facilities were informed immediately,” said the health department authorities, pointing out that immediate testing would occur at these locations.
"We want to nip the virus in the bud," said Health Minister Spahn.
Germany now has the capacity in its labs to carry out up to one million tests a week, Susanne Glasmacher, a spokesperson for the Robert Koch Institute, told The Local.
Of the tests which have been conducted, one percent have come back positive, “a very good result in international comparison,” said Glasmacher.
READ ALSO: Coronavirus outbreak in Germany is 'under control' says health minister
The test capacity in Germany has progressively grown larger since the start of the outbreak. By March 9th, there were 28 laboratories in Germany processing results, with a total of 7,115 tests carried out per week.
By June 15th, Germany counted 138 such labs, and had the capacity to carry out 166,445 tests per day, meaning capacity was nearly twice the number of actual tests being carried out.
But testing only works with tracing and Germany has 400 coronavirus call centres where operators field calls from people worried they might have contracted the virus after coming into contact with a person who tested positive.
They not only put them in touch with medical personnel to arrange for a test themselves, but - working with 21,000 tracers throughout the country - aim to track down every person the positive person has come into contact with and alert them.
Germany is also armed with a new voluntary coronavirus warning app, which can measure whether smartphone users have come closer than about two meters to an infected person for over 15 minutes.
They can then quickly seek out a test.
The success of testing also relies on those people who are positive going into a two-week quarantine, even if they have no symptoms.
Quarantine rules
Germany has strict punishments for those who flout the rules.
Violation of quarantine could in extreme cases result in a maximum prison sentence of up to two years or a steep fine. The health authorities check the quarantine by calling the affected person's home to talk to the patient and check how they are doing.
But not everything is perfect with Germany’s testing strategy.
Despite all of its resources, hotlines and testing centres for the coronavirus often remain closed on weekends, or after hours.
While large metropolitan centres are equipped with several makeshift centres and drive-in testing centres - which can accept patients after they are referred by local health authorities - more rural areas have less resources.
Amr Aswad, a virology researcher at Berlin's Free University, told The Local that the system for testing in Germany was working "very well" but that Germany could make an even greater push to test more asymptomatic people.
"There is a case to be made for testing more asymptomatic people, particularly in situations where a large number of people are gathered, even if they are observing social distancing," said Aswad.
"It's hard to say for sure but I think this could help stop the chain of transmission in its tracks early on."
Testing is 'building block'
The pandemic - and concerns about it - are still far from over in Germany as the recent outbreaks detailed above show.
As of Sunday June 21st, the so-called R-Wert or reproductive value, had shot up from 1.79 to 2.88 following the recent outbreaks.
What’s clear is that Germany, thanks to its well-established testing strategy set up right from the outset, appears well-placed to be able to prevent a second wave.
“Testing is a big building block,” said Schmidt-Chanasit. “It's very important as Germany goes from general blanket measures to specific ones. Testing plays a very important role in ensuring success.”
Schmidt-Chanasit said that such a comprehensive testing strategy of identifying contacts of an infected person - whether co-workers, schoolmates or acquaintances - is the way forward.
“As soon as a contact person arises, there must be a lot of testing,” said Schmidt-Chanasit.
“Now and in the future.”
Join the conversation in our comments section below. Share your own views and experience and if you have a question or suggestion for our journalists then email us at [email protected].
Please keep comments civil, constructive and on topic – and make sure to read our terms of use before getting involved.
Please log in here to leave a comment.