COMPARE: How fast are European countries vaccinating their populations?
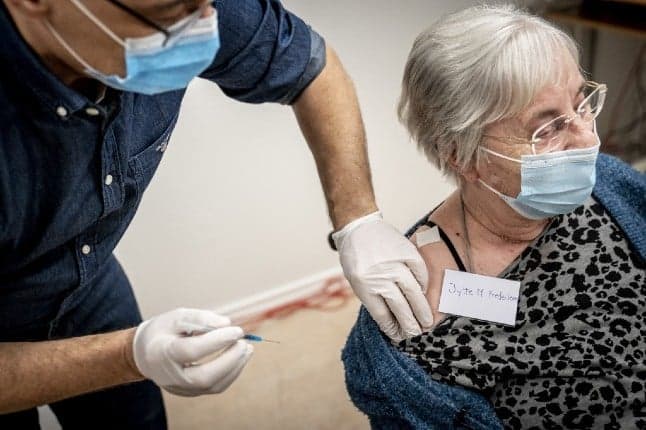
Governments across Europe are hastily vaccinating their populations against the Covid-19 virus as infection rates remain worryingly high. We look at how some countries are having more success than others and the reasons why.
How big a difference is there in the speed of vaccination?
In short, a lot.
Denmark, the fastest country off the mark in the European Union - where rollouts began on December 27th, had given the first vaccine dose to 2% of its population (115,932 people) by January 10th.
Based solely on population share that's ten times the percentage that France - where the government has been heavily criticised for its slow rollout - has managed to achieve. Denmark's SSI infectious diseases agency updates its vaccination statistics daily at 2pm here.
Italy is also pushing ahead rapidly, with 1.2% of the population (654,362 people) having already received the first dose. The country's latest vaccination data, both regional and national, is being continuously updated on this website.
Spain, Sweden and Germany have been slow but steady, with 0.87% (406,091), 0.78% (80,000) and 0.73% (688,782) of the population receiving a jab by January 10th/11th respectively. Spain's data is released here, Sweden's here, and Germany's here.
Norway, Austria, and France, are the laggards of the countries covered by The Local, vaccinating 0.38% (20,833), 0.33% (38,545) and 0.21% (138,351) of their populations respectively by January 10th/11th.
Norway's vaccination data is updated daily here, Austria's is updated in real time here, and France's here.
Switzerland has not yet provided national data on the number of people vaccinated although by the end of next week, it will have had 560,750 vaccination doses delivered, with which 4% of the population can be vaccinated.
All of the above still lie far behind the UK, however, which had managed to give the first dose to nearly 4% of the population - over 2.3 million people - by January 11th. The UK started vaccinating people on December 8th 19 days before EU countries.
Experts say 70 percent of a country's population must be inoculated against Covid-19 in order to end a pandemic that has wreaked social and economic havoc.
As of yet, there's no data on how many, if any of each country's population has received the second dose of the Pfizer-BioNTech vaccine required to get full immunity. Pfizer-BioNTech recommend giving the second dose between 21 and 28 days after the first dose.
What's behind the difference in rates of vaccination?
The main differences seem to come down to a variety of factors including limited stocks of doses and how countries have overcome logistical constraints that come in part with delivering a vaccine that needs to be stored at -70C.
But other factors are also believed to have influenced the pace of rollouts and the strategies behind them including; the level of anti-vaccination sentiment in countries, the extent to which they are concentrating on health personnel (faster) or elderly care home residents (slower), whether countries are choosing to delay the second dose to favour administering more first doses of the vaccine, the extent to which health personnel took time off over Christmas and New Year, and the overall organisation of healthcare systems.
But there have also been some local problems that affected the rollout including historic levels of snow in Spain or problems with delivery. In Bavaria health authorities lost hundreds of doses after taking the unusual step of transporting shipments of the vaccine in camping fridges.
Other states in Germany have blamed problems with difficulty reporting vaccination numbers to a central authority.
Who is saving or delaying the second dose?
Denmark on January 5th said it would now recommend spacing out the two doses of the Pfizer-BioNTech vaccine by six weeks, up from four previously, allowing more people to receive a first injection.
This came after the UK's decision to space out doses by 12 weeks helped it become one of the fastest counties in the world at rolling out its vaccines.
Denmark is not saving the second dose, trusting that Pfizer will deliver as promised.
In Sweden, several of the 21 regions have been storing the second dose, slowing down the roll-out. The public health agency has now advised them not to store the second dose.
In Italy, far from holding doses back, the government is considering rewarding the regions that use up their doses fastest by restocking them first.
In Spain, the plan is to give the second dose to those who have already had their first dose before moving onto the next priority group.
Scepticism
France's extremely slow start has been partly blamed on its over-complicated procedure for consent in care homes, with each patient offered a consultation with a doctor where they are informed of the "benefits and risks of vaccination", and homes given a leisurely two weeks to carry out the process. This has now been reduced to one as the country moved to speed up its roll-out.
 An anti-vax protesters in France. AFP
This is because the high level of scepticism against vaccines has led the French government to take a cautious, some might say overcautious, approach. Some argue that there are other explanations, however.
The high level of openness to vaccination in Denmark is part of the reason the government has felt able to move much faster. A Danish survey found in November that 79% of Danish citizens were willing to be vaccinated, compared to 41% in France, 54% in Italy and Germany, and 50% in Sweden.
Is healthcare national or regional?
Germany's slowish start has been blamed in part to its federal structure, with different states taking a different approach. You can find out about the different states' approaches in our article here.
On the other hand, France's even slower start has been put down to its top heavy, excessively centralised state.
In Denmark's hybrid system, the state has long been responsible for vaccinations, even though the country's five regions are responsible for hospitals and primary care, making the current role out easier to control centrally.
The Christmas effect?
Authorities in Spain blamed the initial slow start of vaccination on the number of health staff who took time off on Christmas and over New Year. Officials in France have similarly blamed the la trêve des confiseurs (the festive lull).
Who is using the extra doses in the vial?
The vials containing the Pfizer-BioNTech vaccine, which are supposed to contain five doses, often contain as many as seven.
While Denmark has been using these from the start, some other countries' health personnel were told to discard the additional doses until the European Medicines Agency on January 8th put out a press release saying the sixth dose can be used.
In Sweden, the national medicines agency only updated its national recommendations on January 11th, after it emerged that several regions were discarding vials after extracting five doses.
An anti-vax protesters in France. AFP
This is because the high level of scepticism against vaccines has led the French government to take a cautious, some might say overcautious, approach. Some argue that there are other explanations, however.
The high level of openness to vaccination in Denmark is part of the reason the government has felt able to move much faster. A Danish survey found in November that 79% of Danish citizens were willing to be vaccinated, compared to 41% in France, 54% in Italy and Germany, and 50% in Sweden.
Is healthcare national or regional?
Germany's slowish start has been blamed in part to its federal structure, with different states taking a different approach. You can find out about the different states' approaches in our article here.
On the other hand, France's even slower start has been put down to its top heavy, excessively centralised state.
In Denmark's hybrid system, the state has long been responsible for vaccinations, even though the country's five regions are responsible for hospitals and primary care, making the current role out easier to control centrally.
The Christmas effect?
Authorities in Spain blamed the initial slow start of vaccination on the number of health staff who took time off on Christmas and over New Year. Officials in France have similarly blamed the la trêve des confiseurs (the festive lull).
Who is using the extra doses in the vial?
The vials containing the Pfizer-BioNTech vaccine, which are supposed to contain five doses, often contain as many as seven.
While Denmark has been using these from the start, some other countries' health personnel were told to discard the additional doses until the European Medicines Agency on January 8th put out a press release saying the sixth dose can be used.
In Sweden, the national medicines agency only updated its national recommendations on January 11th, after it emerged that several regions were discarding vials after extracting five doses.
 The Pfizer-BioNTech vaccine being delivered in the UK. AFP
What are each country's vaccination priorities?
Some countries have initially focused exclusively on those living in elderly care facilities. Others have also prioritised front-line health staff, and others in high risk groups.
Denmark is initially vaccinating residents of retirement homes, the vulnerable over 65s and frontline healthcare workers, according to its strategy announced in November.
Italy is vaccinating 1.4m doctors and nurses first, meaning it has yet to begin giving the jab to the 570,000 residents in elderly care homes. This part explains why it has managed to vaccinate so fast.
France initially started focusing only on very old people, but on January 3rd expanded this to include health workers over the age of 50 in the country's hospitals.
Sweden also began its campaign with a plan to begin by vaccinating only care homes residents, but after heavy criticism from health personnel, on January 5th changed strategy to include frontline health staff as well.
Spain has also begun by focusing on elderly residents in elderly care homes, but is also vaccinating staff at the homes. It aims to have given the first dose to all care home residents by Sunday 17th January.
Second in line are health workers and other vulnerable people such as the elderly and people with underlying health conditions.
Germany started with residents and staff in elderly care homes, but has already begun to offer the vaccine to others over the age of 80, regardless of whether they live in elderly care homes. How this is happening depends largely on state authorities.
Vaccination centres opened in Saarland at the end of December, in Schleswig-Holstein from January 4th, in Rhineland-Palatinate on January 7th, in Saxony on January 11th, and are expected to open in Thuringia from January 13th. Other states are expected to open theirs in the coming weeks. Most states have a phone booking system.
Norway is starting by vaccinating residents in nursing homes and frontline health and nursing staff, including those working in care homes. It will then start to vaccinate those above the age of 85, and further health personnel.
Austria is starting by vaccinating people over the age of 65, and “especially those in retirement and old age homes”, as well as staff in nursing homes.
Switzerland is prioritising risk groups -- the elderly, people with diabetes, chronic lung disease and high blood pressure, and also essential healthcare workers. Second in line are health care workers in daily contact with patients, and those who take care of vulnerable people, including nurses at care homes.
The Pfizer-BioNTech vaccine being delivered in the UK. AFP
What are each country's vaccination priorities?
Some countries have initially focused exclusively on those living in elderly care facilities. Others have also prioritised front-line health staff, and others in high risk groups.
Denmark is initially vaccinating residents of retirement homes, the vulnerable over 65s and frontline healthcare workers, according to its strategy announced in November.
Italy is vaccinating 1.4m doctors and nurses first, meaning it has yet to begin giving the jab to the 570,000 residents in elderly care homes. This part explains why it has managed to vaccinate so fast.
France initially started focusing only on very old people, but on January 3rd expanded this to include health workers over the age of 50 in the country's hospitals.
Sweden also began its campaign with a plan to begin by vaccinating only care homes residents, but after heavy criticism from health personnel, on January 5th changed strategy to include frontline health staff as well.
Spain has also begun by focusing on elderly residents in elderly care homes, but is also vaccinating staff at the homes. It aims to have given the first dose to all care home residents by Sunday 17th January.
Second in line are health workers and other vulnerable people such as the elderly and people with underlying health conditions.
Germany started with residents and staff in elderly care homes, but has already begun to offer the vaccine to others over the age of 80, regardless of whether they live in elderly care homes. How this is happening depends largely on state authorities.
Vaccination centres opened in Saarland at the end of December, in Schleswig-Holstein from January 4th, in Rhineland-Palatinate on January 7th, in Saxony on January 11th, and are expected to open in Thuringia from January 13th. Other states are expected to open theirs in the coming weeks. Most states have a phone booking system.
Norway is starting by vaccinating residents in nursing homes and frontline health and nursing staff, including those working in care homes. It will then start to vaccinate those above the age of 85, and further health personnel.
Austria is starting by vaccinating people over the age of 65, and “especially those in retirement and old age homes”, as well as staff in nursing homes.
Switzerland is prioritising risk groups -- the elderly, people with diabetes, chronic lung disease and high blood pressure, and also essential healthcare workers. Second in line are health care workers in daily contact with patients, and those who take care of vulnerable people, including nurses at care homes.
Comments
See Also
How big a difference is there in the speed of vaccination?
In short, a lot.
Denmark, the fastest country off the mark in the European Union - where rollouts began on December 27th, had given the first vaccine dose to 2% of its population (115,932 people) by January 10th.
Based solely on population share that's ten times the percentage that France - where the government has been heavily criticised for its slow rollout - has managed to achieve. Denmark's SSI infectious diseases agency updates its vaccination statistics daily at 2pm here.
Italy is also pushing ahead rapidly, with 1.2% of the population (654,362 people) having already received the first dose. The country's latest vaccination data, both regional and national, is being continuously updated on this website.
Spain, Sweden and Germany have been slow but steady, with 0.87% (406,091), 0.78% (80,000) and 0.73% (688,782) of the population receiving a jab by January 10th/11th respectively. Spain's data is released here, Sweden's here, and Germany's here.
Norway, Austria, and France, are the laggards of the countries covered by The Local, vaccinating 0.38% (20,833), 0.33% (38,545) and 0.21% (138,351) of their populations respectively by January 10th/11th.
Norway's vaccination data is updated daily here, Austria's is updated in real time here, and France's here.
Switzerland has not yet provided national data on the number of people vaccinated although by the end of next week, it will have had 560,750 vaccination doses delivered, with which 4% of the population can be vaccinated.
All of the above still lie far behind the UK, however, which had managed to give the first dose to nearly 4% of the population - over 2.3 million people - by January 11th. The UK started vaccinating people on December 8th 19 days before EU countries.
Experts say 70 percent of a country's population must be inoculated against Covid-19 in order to end a pandemic that has wreaked social and economic havoc.
As of yet, there's no data on how many, if any of each country's population has received the second dose of the Pfizer-BioNTech vaccine required to get full immunity. Pfizer-BioNTech recommend giving the second dose between 21 and 28 days after the first dose.
 An anti-vax protesters in France. AFP
An anti-vax protesters in France. AFP The Pfizer-BioNTech vaccine being delivered in the UK. AFP
The Pfizer-BioNTech vaccine being delivered in the UK. AFP
Join the conversation in our comments section below. Share your own views and experience and if you have a question or suggestion for our journalists then email us at [email protected].
Please keep comments civil, constructive and on topic – and make sure to read our terms of use before getting involved.
Please log in here to leave a comment.